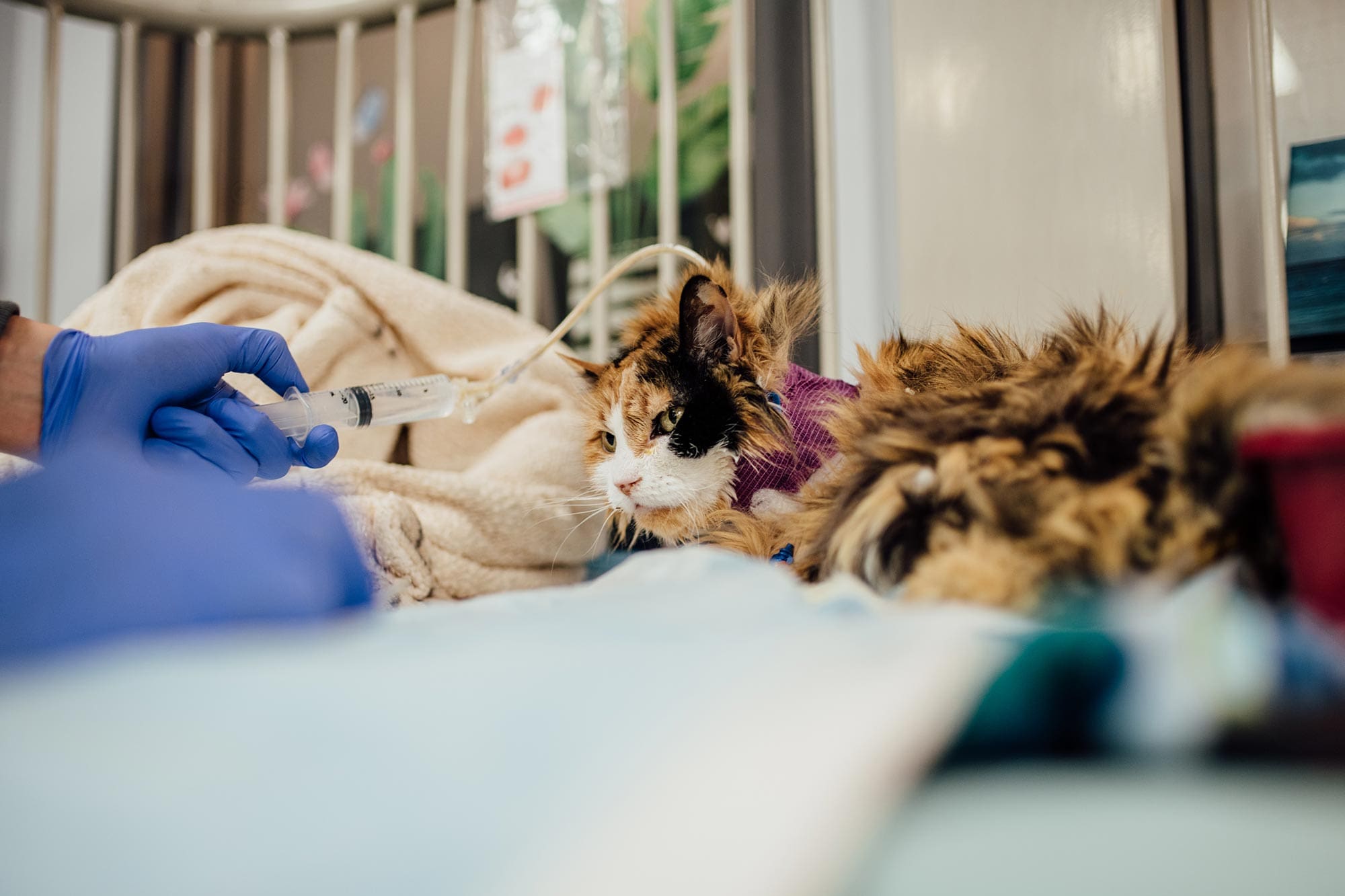
What Causes Evan's Syndrome?
Evan’s syndrome is caused by an abnormal immune response in which the patient’s body targets both red blood cells and platelets for destruction. Primary Evan’s syndrome has no known cause, meaning the immune system was not triggered to attack the red cells or platelets for any identifiable reason. Secondary Evan’s syndrome is suspected when an anemic and thrombocytopenic patient is diagnosed with a new infection or cancer, has recently been started on medication, or received a vaccination that stimulated the immune system. Primary Evan’s syndrome is more common than secondary, but because of differences in therapy and prognosis, a search for an immune trigger is generally recommended.
The immune system has both pro-inflammatory and anti-inflammatory chemical triggers as well as recognition of its own cells; an auto-immune or immune-mediated condition is one in which these mechanisms are deranged. In auto-immune conditions, the full force of the immune response is activated against the body’s own cells. The immune chemicals damage red cells and platelets, causing them to rupture. Damaged cells are removed from circulation by the filtering function of the liver and spleen.
Clinical Signs of Evan's Syndrome


Because platelets are involved in normal blood clotting and red cells are involved in carrying oxygen to tissues, patients with anemia and thrombocytopenia can often be profoundly and acutely ill. They often are pale, weak, and out of breath, and may also have bruises noted in their skin or mouth. Some patients will bleed from the nose or mouth or have blood visible in their urine or feces. Some patients bleed internally and present to the hospital for severe weakness or collapse. Patients in this condition must be evaluated quickly.
Diagnosis
Patients suspected of having Evan’s syndrome are usually diagnosed with a combination of blood tests and imaging studies (radiographs/X-rays and ultrasound). Blood tests generally show anemia and low numbers of platelets from the immune system attack. Patients often have elevated white cell counts from the immune stimulation and may also have abnormal organ function tests from the stress of the anemia and low platelets on other organs.
To look for causes of secondary Evan’s syndrome, patients who are severely anemic and thrombocytopenic generally have blood tests to look for infectious causes of low platelets. In dogs, these are usually diseases that are carried by ticks; in cats, screening tests for bacterial and viral causes of anemia or thrombocytopenia are generally done. Because cancer can trigger an aberrant immune response, radiographs (X-rays), ultrasound, and sometimes bone marrow analysis are recommended as well.
Treatment
Depending on the severity of your pet’s condition, hospitalization for fluids, supportive care, and transfusions may be necessary.


Evan’s syndrome is treated with medications that attenuate or calm the immune system. Steroids are frequently used in addition to other immunomodulating drugs.
It is not uncommon for more than one immunomodulatory medication to be necessary to gain control of the disease. Patients with Evan’s syndrome associated with an infection may need medication to treat the infection. Patients who develop Evan’s syndrome secondary to cancer may be treated with chemotherapy, surgery, or other disease-directed therapy.
Plasma exchange or plasmapheresis is a newer therapy available to treat the most severe cases of immune-mediated disease. Therapeutic plasma exchange (TPE) involves exchanging the plasma component of the patient’s blood with that of a healthy plasma donor. The patient’s blood is circulated through a filter (similar to kidney dialysis) to allow the sick patient’s plasma to be cleaned of the destructive circulating immune chemicals while preserving as many red blood cells and platelets as possible. Because some of the patient’s plasma is removed in the process, a donor’s plasma must be returned to the patient during the exchange process. This therapy is available at Veterinary Specialty Center.

What is the Prognosis for Evan's Syndrome?
Evan’s syndrome is a life-threatening disease, more serious than either immune-mediated thrombocytopenia or anemia on their own, but some patients do respond to immunosuppressive medications and aggressive supportive care. Patients who require transfusions in the first few days of therapy have a more dangerous form and are likely to need more hospitalization for several days.
The first few days after Evan’s syndrome diagnosis are the most dangerous and some patients do not respond to aggressive therapy. A patient who survives the first several days of therapy and is discharged from the hospital generally has a good long-term prognosis, although close monitoring is necessary.
Patients with secondary Evan’s syndrome, associated with infection or cancer, can have a variable prognosis, depending on the inciting cause.
Long Term Follow-Up
Patients with Evan’s syndrome are followed by the internal medicine specialists at Veterinary Specialty Center. Our doctors always keep primary care veterinarians informed about each patient’s medical condition and therapeutic plan. Close monitoring, especially in the early phase of the disease, is critical. Discontinuing medications too soon can result in a relapse of inflammation, and relapses tend to be more severe than the initial onset of the disease. Medication dosages should never be reduced unless recommended by the veterinarian who has managed the disease. Additionally, patients must be monitored for medication side effects. In general, the goal is to reduce medication to the lowest effective dose. It may take months and many visits to achieve long-term control of a patient with severe or relapsing Evan’s Syndrome.
Because decisions about changes in medication are based on observations made during the physical exam in addition to other testing, we recommend that follow-up for this disease is done at Veterinary Specialty Center. Future vaccination is often not recommended but all other routine preventive care should continue with your primary care veterinarian.
Remember that Veterinary Specialty Center never closes, do not hesitate to come in or call if you are concerned about your pet.