It can often be challenging to diagnose and manage some of your pet’s medical conditions. Certain illnesses require more advanced diagnostics, may not be responding to traditional treatments, or may be rare and difficult to diagnose. In these situations, your pet may need to be evaluated by an internist, a veterinarian who specializes in veterinary internal medicine–the diagnosis and treatment of internal diseases.
Veterinary Specialty Center’s experienced veterinary internal medicine specialists are ready to help with any complex cases. Our doctors and their teams are dedicated to caring for dogs and cats with chronic, serious, and life-threatening illnesses. They collaborate with each other and also work closely with our cardiology, oncology, surgery, clinical pathology, and emergency and critical care specialists to arrive at a diagnosis and create a comprehensive treatment plan for your pet.
VSC is also at the forefront of treating pets with kidney disease in the United States. We are one of the few veterinary hospitals that offer hemodialysis and plasmapheresis, which expand our treatment options for kidney disease, immune-mediated illnesses, and toxicity cases.
What to Expect at Your Internal Medicine Appointment


Our board-certified internal medicine specialists assess patients with complex medical issues that involve multiple body systems, focusing on metabolic, immune-mediated, and infectious diseases that are difficult to manage and require advanced diagnostics, monitoring, and therapies.
Your internal medicine appointment starts with a consultation, which includes:
-
A physical examination of your pet
-
A discussion about any pertinent history
-
A review of all your pet’s medical records (provided by your primary care veterinarian)
Additionally, your dedicated internist will talk with you about your pet’s condition, any diagnostic tests needed and performed, treatment options, and prognosis. Before doing any treatment, your internist will provide you with a patient care plan.
Conditions Our Internal Medicine Specialists Can Treat
VSC’s skilled internists can diagnose and treat a vast number of internal conditions in dogs and cats, including:
Endocrine Diseases
-
Addison's Disease
-
Cushing's Disease
-
Diabetes
-
Hyperthyroidism
-
Idiopathic Hypercalcemia
-
Pancreatitis
Gastrointestinal (GI) Diseases
-
Gastrointestinal and Esophageal Foreign Bodies
-
Inflammatory Bowel Disease
-
Inflammatory Stomatitis
-
Megaesophagus and Esophagus Dysmotility
-
Perianal Fistulae (PAF)
Hepatic Pancreatic Diseases
-
Hepatic Lipidosis (Fatty Liver Disease)
-
Portosystemic Shunts (PSS)

Immune-Mediated Diseases
-
Immune-Mediated Hemolytic Anemia (IMHA)
-
Immune-Mediated Polyarthritis (IMPA)
Infectious Diseases
-
Babesia
-
Blastomycosis
-
Leptospirosis
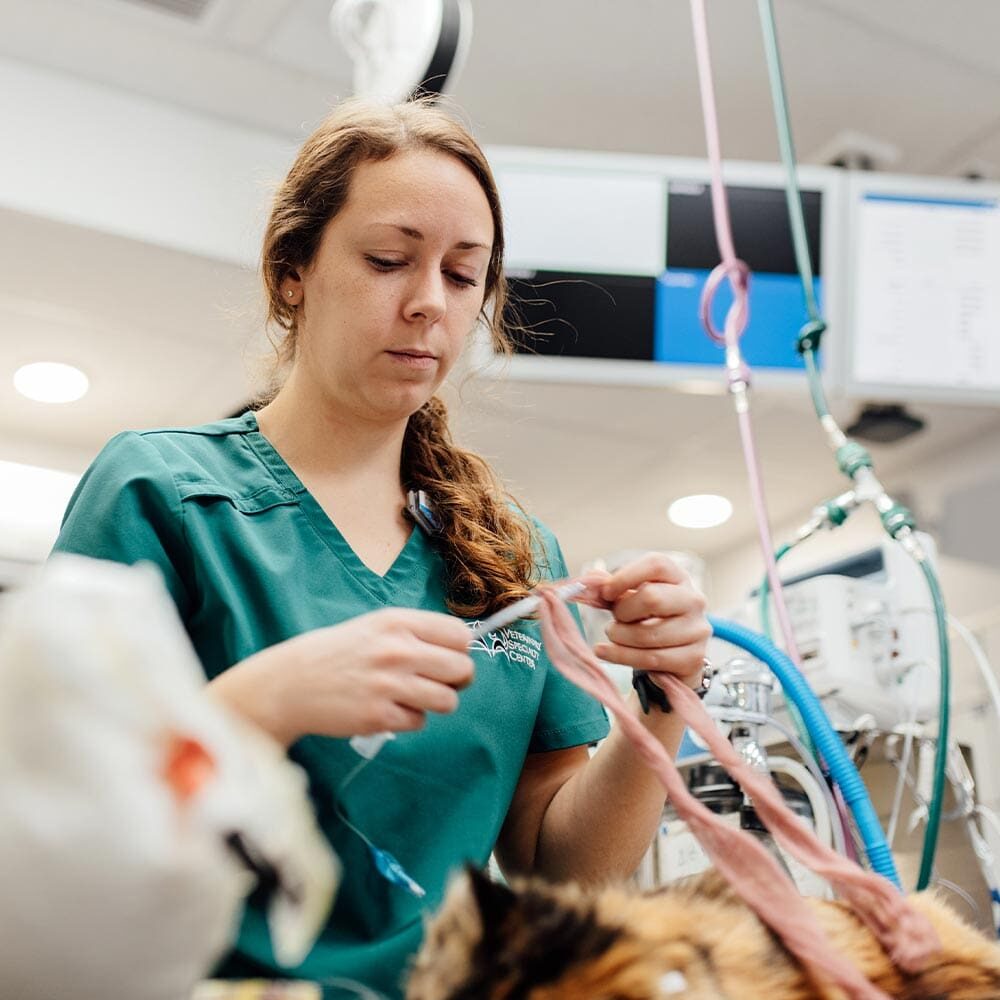
Procedures We Perform
Our Internal Medicine Department provides the following services:
Scopes
-
Gastrointestinal Endoscopy
-
Cystoscopy
-
Bronchoscopy
-
Rhinoscopy
-
Bone Marrow Aspirates
Feeding Tubes
-
Esophagostomy
-
Percutaneous Endoscopic Guided (PEG)
Fluid Tests
-
Cerebrospinal Fluid Tap (CSF)
-
Complete Blood Count (CBC)
-
Serum Chemistry Profile
-
I-STAT
-
Coagulation Tests
-
Arterial/Venous Blood Gas
-
Urinalysis
-
Immune
-
Infectious Disease
-
Endocrine
-
Joint Taps

