What Causes PLE?
The cause of PLE can be an inflammatory condition (sometimes referred to as IBD), intestinal cancer, or severe parasitic infection. Any disease that disrupts the normal intestinal wall function can cause protein-losing enteropathy. Other times, non-GI causes such as liver disease or heart disease can cause PLE.


Clinical Signs
Most patients with protein-losing enteropathy have signs of gastrointestinal dysfunction such as vomiting, diarrhea, weight loss, and poor appetite. The severity of the protein loss varies from patient to patient. Because alterations in blood protein can cause vascular leakage, some patients have fluid accumulation in the abdomen or chest cavity, making them appear bloated or causing breathing problems. Some milder affected patients have no clinical signs and the abnormality is detected in blood work.
Diagnosis
Diagnosis
Protein-losing enteropathy is a term that describes the disease but is not a true diagnosis. The only way to determine the diagnosis or cause of the intestinal malfunction is to do a biopsy of the affected portion of the intestinal tract.
Without a biopsy, the cause of your pet’s protein-losing enteropathy (PLE) will be unknown. In almost every patient, we recommend doing a biopsy of the intestine to determine the cause of the protein loss. Because some patients with PLE are profoundly ill, we have to consider the risks of anesthesia and the procedure against the risks of treating without an accurate diagnosis.

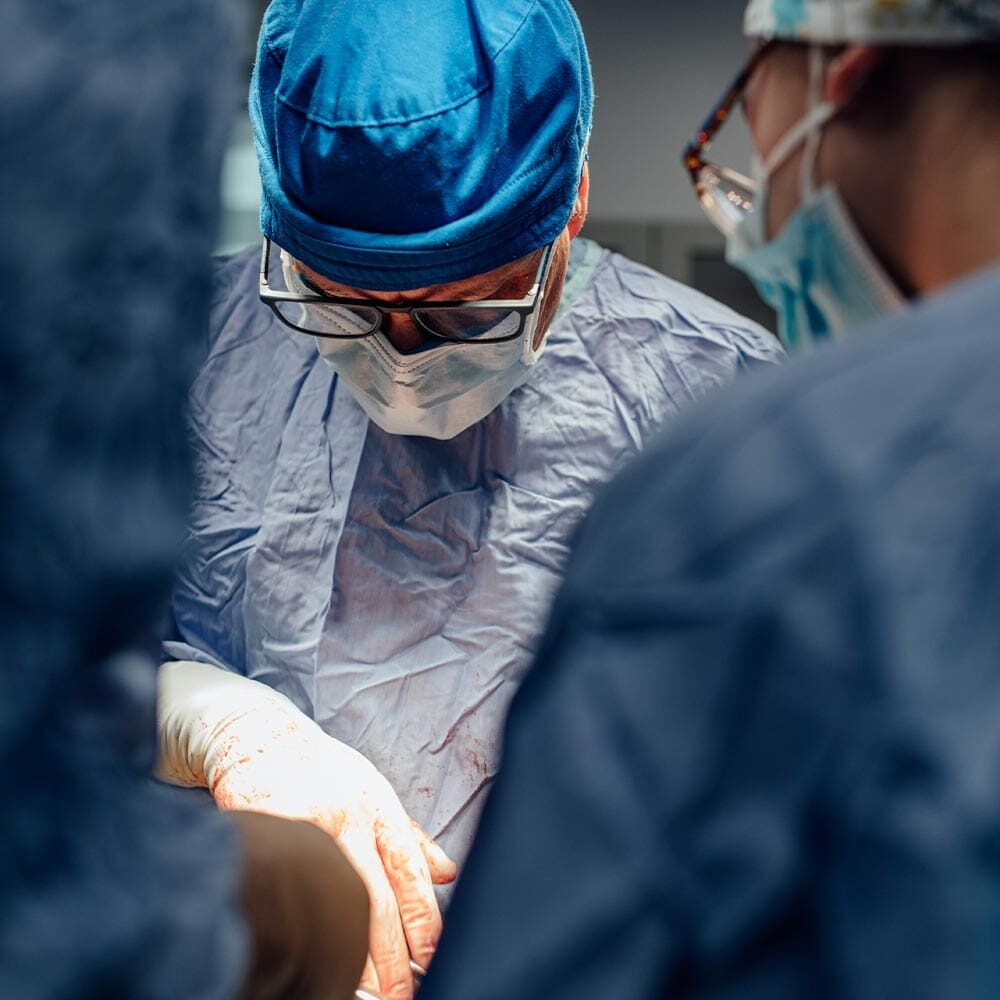
The biopsy options available are either an endoscopic biopsy or a surgical biopsy.
An endoscopic biopsy is a less invasive test but does require general anesthesia. For an endoscopic biopsy, a video scope is used to better visualize the stomach and small intestines, and small biopsies are obtained for sampling. The advantage of this procedure is that this is a non-invasive, outpatient procedure. The disadvantage is that the camera may not extend far enough into the intestines to allow a full examination of the intestinal disease, and biopsies obtained are of the superficial, internal layers only.
The other alternative is a full-thickness surgical biopsy. This allows a more thorough assessment, however, is also more invasive requiring anesthesia and abdominal surgery. This test is a more reliable test to evaluate problems in the middle of the intestine (jejunum).
Treatment
Therapeutic recommendations are driven by the results of the biopsy and often include dietary changes, medications to modulate an over-zealous immune response, chemotherapy if indicated, and supplements.
Empiric therapy – meaning treatment that is started without obtaining a biopsy is sometimes chosen after a discussion of risks and costs. It is important to note that empiric treatment has some potential risks. Starting medications before obtaining a diagnosis may result in an alteration of the disease state which makes it more difficult to obtain accurate biopsy results in the future. Still, because some patients are quite ill, making anesthesia and biopsy procedures risky, empiric therapy is preferable to putting the patient at risk.
Empiric treatment would consist of supportive care, which can include transfusions of plasma (protein), fluids to help electrolyte abnormalities, anti-nausea and anti-diarrheal medications, vitamin B12 injections, diet changes (low fat and hydrolyzed or hypoallergenic), and often steroid medication. Other treatments sometimes include an antibiotic or an anti-parasitic medication. If there is an incomplete response or no response in the first few days or weeks of this therapy, often a more potent oral immune-modulating medication may be prescribed.
For patients who are being treated without a biopsy, we must carefully consider the possibility of a cancerous condition when we are treating with potent immunomodulators. Although inflammatory/immune-mediated causes of intestinal disease are more common than cancer, when treating without a biopsy-confirmed diagnosis, there will always be a risk that medications could harm the patient.
Prognosis
The prognosis for patients with PLE depends upon the underlying cause. When the cause is an aberrant immune response, the majority of patients can be controlled with medications, diet, and some supplements.
Patients who develop PLE due to intestinal cancer have a variable prognosis. Some can be controlled with a good quality of life for months or years with chemotherapy medications and others decline within weeks.
It is important to note that it can take some time for patients to respond to therapy. A significant challenge is that the medications we are using to treat the disease must be absorbed by the poorly functioning intestinal tract. Even with accurate biopsy results driving medication decisions, some patients do not tolerate the recommended medications or diet and there can be a frustrating period of trial and error.
Long-Term Follow-Up
Long-Term Follow-Up
Patients with PLE are generally diagnosed and treated by the internal medicine specialists at Veterinary Specialty Center. Depending on the cause of PLE and the therapy recommended, many patients require monitoring of lab tests and progress. Prednisone, which has significant long-term side effects is generally tapered off within the first few months. Additional immune-modulating medication dosages can often be tapered over time when the disease is under control. Because immune-modulating medications have potential side effects, monitoring is necessary to keep the patient safe. Some patients can achieve control, be tapered off all medications, and maintain on diet and supplements only, reducing the need for follow-up with a specialist.