Radiation Therapy – Mast Cell Tumors
 Mast cell tumors (MCT) are very common in dogs but extremely rare in humans. Mast cells are a special type of blood cell that is normally involved in the body’s response to allergens and inflammation. MCT can look and feel like anything, so it is impossible to know if a skin mass is an MCT without looking at cells under the microscope. MCTs are generally thought of as malignant tumors that have the ability to regrow if they are incompletely removed, and some may spread to other organs.
Mast cell tumors (MCT) are very common in dogs but extremely rare in humans. Mast cells are a special type of blood cell that is normally involved in the body’s response to allergens and inflammation. MCT can look and feel like anything, so it is impossible to know if a skin mass is an MCT without looking at cells under the microscope. MCTs are generally thought of as malignant tumors that have the ability to regrow if they are incompletely removed, and some may spread to other organs.
Mast cells contain reactive substances that can be released into the bloodstream and potentially cause inflammatory effects. These might include stomach ulcers, bleeding, and/or allergic reactions (anything from swelling around the tumor to life-threatening shock). When an MCT is diagnosed and is widespread, we often prescribe anti-inflammatory doses of steroids, GI protectants, and antihistamines to mitigate these effects. While getting a sample of the mass with a needle can give us a diagnosis, we require a biopsy in order to determine how aggressive we might anticipate a tumor could act. This measurement of aggressiveness is called a “grade”. Low-grade, (grade 1 or low-grade 2) tumors often do not spread beyond the skin mass, while high-grade (some grade 2 or grade 3) are more prone to spreading to other organs (metastasis). Different locations of an MCT can also act more or less aggressive in general. Local therapy may be the only treatment required for low-grade tumors, such as surgery and/or radiation, while it is recommended to combine local therapy with chemotherapy for high-grade tumors.
If an MCT can be removed with complete, or clean, surgical margins, this may be all the treatment required locally. Low, grade 1 MCT uncommonly grow back even with incomplete surgical margins (7% risk of recurrence), so they are often just monitored over time. However, some tumors are not amenable to complete surgical resection, leading to incomplete, or “dirty”, surgical margins, or there is no surgical option at all.
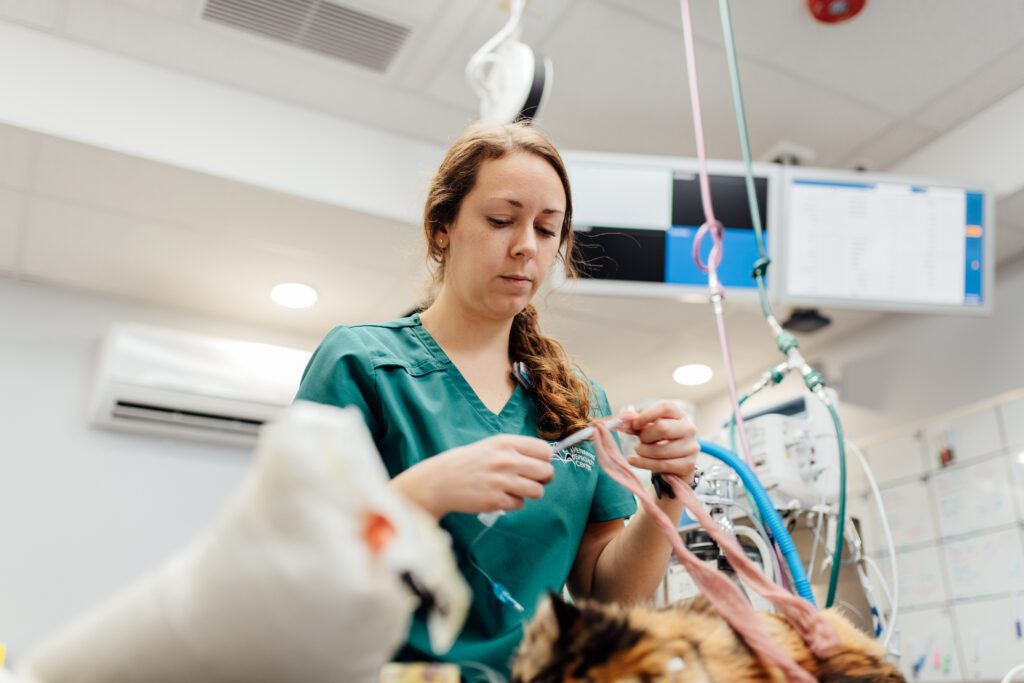
Radiation therapy can be combined with incomplete surgical resection in many cases. This consists of 15 treatments of radiation daily, Monday through Friday. The radiation is delivered via a machine called a linear accelerator (LINAC), and single or multiple beams of radiation are directed and centered on the tumor. The patient is anesthetized for a brief time for each of these treatments, usually between 30-45 minutes, and just “deep” enough that they lay still. There is no pain associated with the delivery of radiation itself. Radiation is most effective when the tumor cells remaining are in a microscopic setting (such as after surgery). With this protocol, approximately 90% of dogs will respond to treatment and live for 2+ years without evidence of tumor regrowth.
If the tumor is found on the chest or abdomen, sometimes a computed tomography (CT) scan is required for more targeted radiation planning. Side effects relating to this protocol of radiation are most commonly on the skin. About 2 weeks into the protocol, we can see hair loss, redness or irritation to the skin, and by the end of the protocol, we often see skin ulcerations. These side effects may get worse up until about 1-2 weeks after completing the radiation protocol, then in the majority of patients, heal over the next couple weeks with no long-term complications. Keeping the region of radiation side effects clean, dry, and uninfected (no licking, biting, or rubbing by the patient) is the best way to ensure appropriate healing.
Finally, we can irradiate MCTs in the gross setting with a hypofractionated (“hypo” meaning “low” or “few” number of treatments) radiation protocols. These protocols are not as aggressive as the two previously mentioned options, however, there is some literature available that these protocols, with or without certain medications, can have good tumor responses. One publication reports a median survival time of about 1 year following treatment with this protocol and chemotherapy called Palladia (toceranib). Another publication estimated median control times at 2+ years for low-grade tumors when treated with radiation and prednisolone (a corticosteroid). These studies were performed on gross MCT and the radiation was delivered weekly for 4 weeks, taking week 3 as a break (sometimes called the 0, 7, 21 protocol for the days on which radiation is administered). Other protocols entail daily radiation for 5 days – Monday through Friday – or radiation once a week for 6 weeks. We believe the efficacy is similar between these protocols, with similar control of the tumors, however, consult with the radiation oncologist to see if one protocol might be preferred for your individual pet. The risk of any side effect is low, since this is a moderate dose of radiation whose intent is to prolong a good quality of life.
The side effects associated with these palliative protocols are much lower, both in severity and frequency. Many patients can complete a protocol and not experience any side effects, however, this risk is never zero.
Thank you for considering bringing your pet to us for treatment. We understand and value the trust you have placed in us. Should you have any questions regarding radiation therapy for the treatment of canine mast cell tumors, please do not hesitate to ask to be put in contact with a member of our radiation oncology team.
